This week a study by Stein and colleagues was published in the New England Journal of Medicine featuring differences in asthma risk between genetically similar Amish and Hutterite children living in the US. The main difference between these two farming groups is their exposure to farm animals. Amish have single family dairy farms and live in close proximity to their animals. By comparison, the Hutterites farm on communal highly industrialized farms. That difference may be enough to protect Amish children from allergies. 1 in 20 Amish kids get asthma, while 1 in 5 Hutterite children have asthma.
I describe the study in the EvolutionMedicine ‘cast #5 Amish Asthma:
What is the agent that protects Amish kids from asthma? Microbes. Amish farming lifestyle makes them have relatively greater exposure to farm animal microbes and antigens.
In this respect the Amish are like the Karelians, a Russian group of traditional farmers with a markedly lower allergy risk compared to genetically similar Finns.
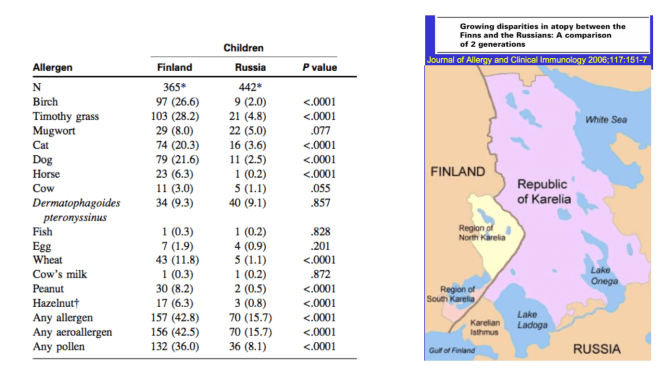
So these associations are not exactly new. What is different about this study is that they showed that the Amish children develop their immune systems differently, with more neutrophils and fewer eosinophils. Neutrophils are innate immune cells that chiefly fight bacterial infections, while eosinophils are immune cells responsible for defense against helminths and are the cells responsible for type 1 hypersensitivity reactions, like asthma. The gene expression patterns of white blood cells in Amish vs Hutterite were also markedly different:

Circulating immune cells had different gene expression patterns in the Amish (blue) compared to the Hutterites (red). These differences are developmental and entirely driven by differences in microbial exposure. Remember, Amish and Hutterite have almost the same ancestors, and are thus remarkably genetically similar. So all these differences, in immune cells and in asthma phenotype, are essentially environmental. The dramatic differences in gene expression seen above is a good example of a human reaction norm (discussed in previous posts like this one). I propose that these changes in immune cell development, and the responses to microbial signals described in the Stein paper, evolved because they were adaptive in historic environments. This idea is similar to the hygiene hypothesis, which uses evolutionary principles, including gene environment mismatch to explain why more autoimmune diseases occur when microbes and pathogens are absent.The hygiene hypothesis was invoked to explain the inverse relationship between childhood infections and autoimmune disorders seen below:
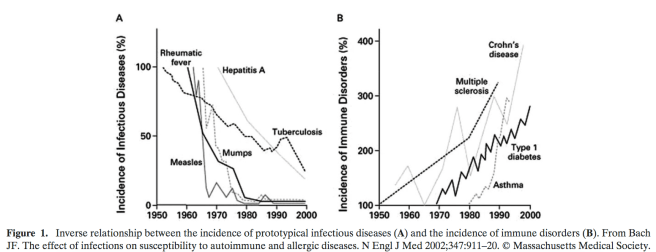
What we don’t know is what kind of microbial exposures, and which route, are most important in determining asthma and allergy risk. In the NEJM study, Stein et al. showed that protection from airway hypersensitivity could be achieved when dust from Amish homes was instilled into the noses of experimental mice. So maybe nasal inoculation of house dust is the most important route exposure. That makes sense since airway exposure would be expected to affect the risk of asthma, an airway disease. But other studies suggest the oral and gut route are important. For instance, Hesselmar and colleagues have looked at pacifier cleaning methods in relation to allergy:
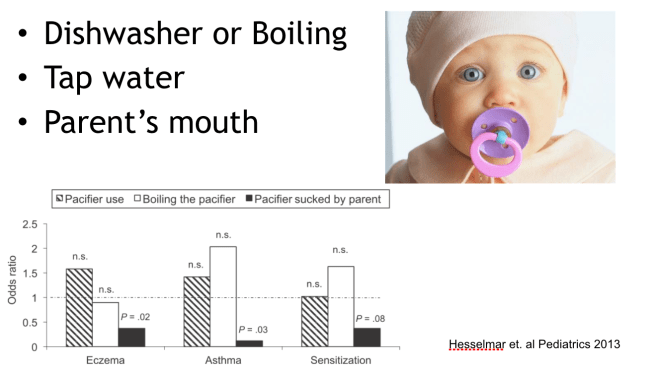
Kids whose parents “clean” their pacifiers by sticking it in their mouth first had fewer allergies, even more so if the child was also born vaginally instead of by c-section. The same group has also shown that owning and using a mechanical dishwasher in the home increases the risk of allergy and asthma.
All of which is to suggest that childhood exposure to microbes, even some potentially dangerous ones, may do more good than harm. Perhaps your child really should “Eat Dirt” as the title of a recent book by Brett Finlay and Marie Claire Arrieta advises.
Here is some final food for thought: even though it horrifies parents, children may be well adapted to sample their microbial environment by putting anything and everything in their small mouths.
Link to New York Times article on the Amish asthma results.
Categories: Microbiome podcasts
Joe Alcock
Emergency Physician, Educator, Researcher, interested in the microbiome, evolution, and medicine

Leave a comment