The New Year is here, and the pale sun may only make a brief appearance, if at all. We normally get vitamin D from the sun, with a lesser contribution from diet, so you may ask yourself – should I be taking vitamin D? In our culture, we are exhorted to “take your vitamins.” A substantial industry promotes the testing and sales of vitamin D. Vitamins and other supplements comprise a $30 billion market. Half of Americans take them, despite little to no evidence that supplements work for healthy children or adults.
A recent nail in the coffin of vitamin supplementation was published in the New England Journal of Medicine. This was an ancillary analysis of a large randomized controlled trial of vitamin D, the VITAL study. VITAL originally aimed to find out whether vitamin D and omega-3 fatty acid supplementation decreased the risk of cardiovascular disease and cancer in healthy older adults who were not screened for low vitamin D levels (spoiler, they don’t). In the recent NEJM paper, the authors wanted to find out whether vitamin D supplementation had any effect on bone fractures. This is an important question since many people take vitamin D believing it will help prevent osteoporosis and fractures. The recent study suggests that vitamin D supplementation is unhelpful for fractures.
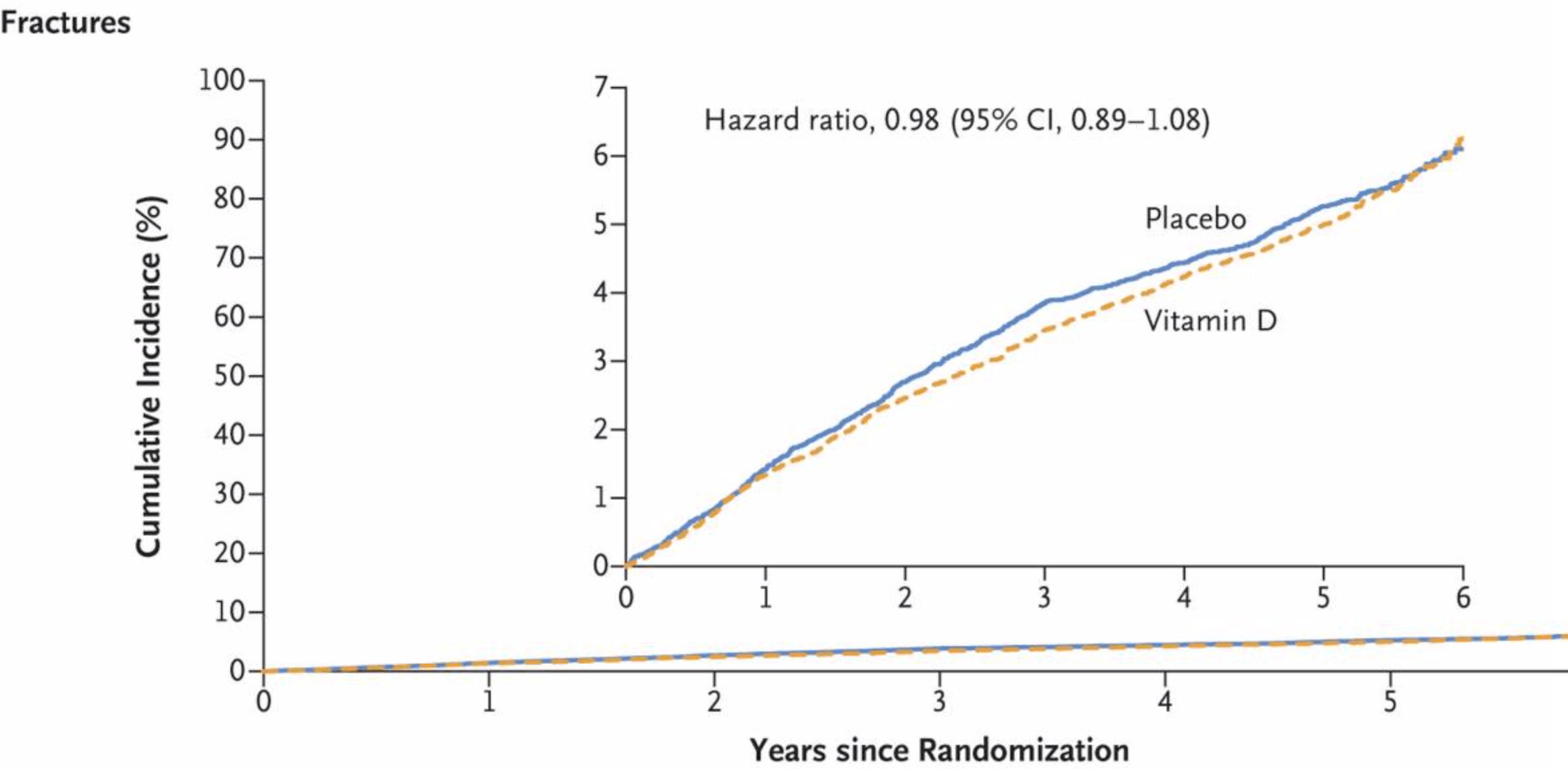
In an editorial accompanying the VITAL study titled VITAL Findings – a decisive verdict on Vitamin D supplementation, Cummings and Rosen wrote “VITAL and this ancillary study show that vitamin supplements do not have important health benefits in the general population of older adults, even in those with low 25-hydroxyvitamin levels (emphasis added.)
They go on: “Results of analyses from VITAL published in peer-reviewed journals have shown that vitamin D supplementation did not prevent cancer or cardiovascular disease, prevent falls, improve cognitive function, reduce atrial fibrillation, change body composition, reduce migraine frequency, improve stroke outcomes, decrease age-related macular degeneration, or reduce knee pain.” Outside of specific risk groups, Cummings and Rosen argue that the terms “vitamin D ‘insufficiency’ and ‘deficiency’ should now be reconsidered.”
This gets me to my next point – when trials don’t work as expected, there is often an evolutionary reason for it. (The same, of course, is true when trials do work.) One reason is that we don’t yet know what is “normal” for vitamin D and its regulation.
Several of the authors of the expert panel that established the threshold limit for normal levels of vitamin D now disavow the panel’s recommended 20 ng/ml threshold.
What is a normal vitamin D threshold level? It is uncertain, but it could be as low as 12.5 ng/ml, which the authors of Vitamin D deficiency – Is there a pandemic? propose. By using 12.5 ng/ml, only about 6% of the population would be deficient (still too many in my view). We don’t know how many in that category would benefit from supplementation.
A deficiency syndrome of vitamin D exists. It is called rickets, and it is caused by an extreme deprivation of vitamin D and calcium in the diet. Rickets historically caused bowing of the legs, because of softening of long bones, or osteomalacia. Most modern vitamin D deficiency is not that, and just because supplementation treatment regimens worked for rickets does not mean that supplements will work for the modern epidemic of vitamin D deficiency.
VITAL throws conventional wisdom on vitamin D into question. It raises the possibility that low vitamin D is less problematic than commonly understood – more a marker than a cause of disease. More speculatively, low vitamin D might be a functional regulated trait. It is widely understood that Vitamin D regulates the immune system, e.g. by adjusting the production of inflammatory cytokines. Although it seems semi-subversive to say it, sometimes inflammation can be a good thing. Also, sometimes, less inflammation is a good thing. By modulating immune responses, the adaptive regulation of 25-hydroxyvitamin D and the vitamin D receptor can have utility for an organism.
Leaving aside the question of whether low vitamin D might be helpful, it never made sense to me that widespread deficiency would be epidemic today. This is especially true in a modern population that has access to adequate vitamin D in the diet. North Americans live in a world in which all milk is fortified and other fortified foods include cereal, juice, bread, yogurt, and cheese.
Cummings and Rosen say it best: “What are the implications of VITAL? The fact that vitamin D had no effect on fractures should put to rest any notion of an important benefit of vitamin D alone to prevent fractures in the larger population. Adding those findings to previous reports from VITAL and other trials showing the lack of an effect for preventing numerous conditions suggests that providers should stop screening for 25-hydroxyvitamin D levels or recommending vitamin D supplements, and people should stop taking vitamin D supplements to prevent major diseases or extend life.”
Oh, and by the way, Vitamin D supplements are not helpful in preventing COVID-19, either.
Most of us, then, can safely stop visiting the vitamin and supplement aisle. Even in the bleak mid-winter, it seems we can set aside our worries about a deficiency, that apparently, does not exist.
Categories: Uncategorized
Joe Alcock
Emergency Physician, Educator, Researcher, interested in the microbiome, evolution, and medicine
Curious why you neglected to cite this study that showed a very significant benefit of vitamin D in preventing Covid.
https://pubmed.ncbi.nlm.nih.gov/35487792/
Thanks for pointing out that study. But that one had a small sample size, which increases the risk of a type 1 error. The studies described in the link involved thousands of patients and the result (probably) is more reliable.