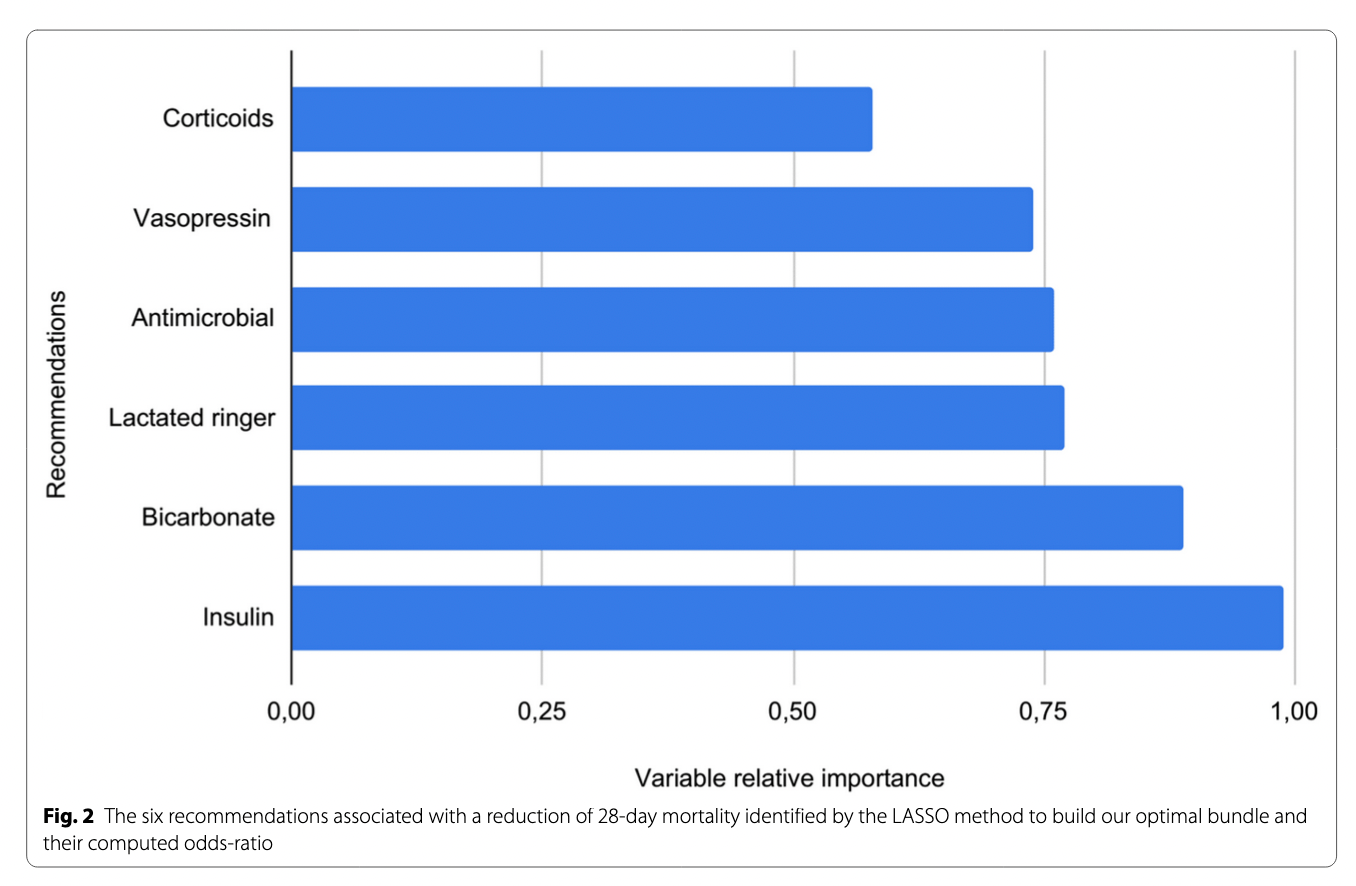
A recent study by Kalimouttou et al. used machine learning to conclude that insulin is one of the most effective interventions to promote survival in sepsis.
The reaction on Twitter included this from Josh Farkas:
Why the laugh emoji? Isn’t machine learning the best way to wade through big data? Isn’t insulin a key treatment for sepsis, since the first care bundle was proposed by the surviving sepsis campaign? You’d be forgiven for believing that insulin is important….if a time machine transported you back to the early 2000s when the New England Journal of Medicine published a report by Van den Berghe supporting the use of an intensive insulin protocol. As Van den Berghe et al. commented in 2007: “Recently, the concept that stress hyperglycemia in critically ill patients is an adaptive, beneficial response has been challenged. Two large randomized studies demonstrated that maintenance of normoglycemia with intensive insulin therapy substantially prevents morbidity and reduces mortality in these patients.”
But subsequent research that involved far more patients in studies that were better designed (multi-center versus single center trials) contradicted the results of the studies Van den Berghe cited. A NEJM paper in 2008 showed harm from giving more insulin: Intensive insulin therapy in sepsis caused more complications with no survival benefit. This was followed by the NICE-SUGAR study that tested intensive insulin treatment, also called tight glycemic control, in 6000 adult critically ill patients. Unexpectedly, NICE-SUGAR showed that tight glycemic control increased mortality by 2.6%. Agus et al followed up on this result in a pediatric study of tight glycemic control in the intensive care unit. This study, published in the New England Journal in 2017, was stopped early because it also showed a signal of harm.

Since then, a meta-analysis by Chen et al. concluded that intensive insulin treatment showed no benefit in critical illness, but that it does increase the rate of hypoglycemic adverse events. Similarly, Arabi showed no benefit of intensive insulin in the adult ICU. We can conclude from these studies that insulin can be harmful. It should be used cautiously, if at all, in critically ill patients. And it’s not just in sepsis that insulin has proven to be worrisome. Studies have shown harm from insulin use in other conditions. Notably, Covid-19 patients die more often when treated with insulin. Chronic treatment of type 2 diabetics with insulin compared to other anti-diabetic treatments is also associated with increased complications, including death.
To recap: Adults in the ICU die more often when given more versus less insulin. Children with critical illness have worse outcomes when treated with intensive insulin. Patients with severe COVID-19, which resembles sepsis in many respects, are more likely to die when treated with insulin.
These and additional lines of evidence tell us that insulin treatment should be de-emphasized in sepsis treatment. There is a good chance that following the advice of Kalimouttou et al‘s machine learning approach would lead to more deaths, not fewer. (And we have not even touched on the other elements of “care” identified in this analysis – the second best intervention in the machine learning analysis, bicarbonate, is almost certainly useless in sepsis.)
Why is intensive insulin treatment a problem? The conventional medical explanation is that insulin treatment results in hypoglycemia. Hypoglycemia is a well-documented adverse consequence of intensive insulin treatment that can cause cardiovascular instability, seizures, coma, and even death. But hypoglycemia by itself cannot explain all the harms of insulin use. Historically, elevated blood sugar after the acute stress of trauma or infection was deemed to be normal – something that didn’t need fixing. Marik and Bellomo wrote in 2013: “hyperglycemia and insulin resistance in the setting of acute illness is an evolutionarily preserved adaptive responsive that increases the host’s chances of survival.” Does the accumulating evidence of insulin’s harm vindicate the view of stress hyperglycemia as a protective, adaptive, response? Probably yes, but we still need to identify what part of the response is beneficial. Is it conserving resources, prioritizing glucose delivery to critical tissues unaffected by insulin resistance? Might it have less to do with blood sugar and more to do with an insulin-mediated CD8+ T cell effect, as Wensveen et al. proposed? Alternatively, Legrand and I wrote our immune brinksmanship paper:
“while cytokine-induced insulin resistance could make glucose available to immune cells (as suggested by Straub et al. 2010), it simultaneously reduces glucose availability to infected cells.”
In that paper, we highlighted competition for glucose between infected cells and immune cells as a driving force in insulin resistance. We suggested that nutrient-starved infected cells are eliminated faster because of the acute phase response and insulin resistance. This idea needs elaboration and prospective testing. As for machine learning, I’m not impressed. Our AI overlords will have to try harder next time.
Categories: Uncategorized
Joe Alcock
Emergency Physician, Educator, Researcher, interested in the microbiome, evolution, and medicine
Another very informative post! I wonder why few–if any–have searched for what impact modulating insulin has on the total system? I think it is an over-simplification to think that insulin is only controlling blood glucose and energy balance. (For instance, insulin, independent of energy partition, has a very powerful impact on essential fatty acid metabolism, which modifies the production and function of pro-resolving mediators.) The potential number of mechanisms that insulin is involved in, or control, is enormous and may be impossible to fully understand–it doesn’t seem that AI is there yet. I guess it is just hard to “fool Mother Nature” and come up with a [better] plan.
Thank you Fred. I agree that insulin’s effects are myriad. Energy is an important part of the story, but not the only one.