Update: a research study performed by Abou-Jaoude and colleagues presented on November 16th at the American College of Allergy Asthma and Immunology examines the link between maternal “mouth cleaning” of infant pacifiers and allergy. They found that “parental pacifier sucking was linked with suppressed IgE levels” in infants. Lower IgE is related to reduced risk of allergic diseases, including atopy and asthma. This work builds on the study by Hesselmar and colleagues that I describe below. Read on:
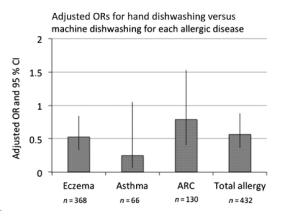
A study by Hesselmar and colleagues in the journal Pediatrics suggested that hand washing dishes may possibly affect allergy risk in children. This observational study involved about 1000 Swedish children. Kids whose parents used an automatic dishwasher had an increased risk of developing allergy and asthma. Handwashing was associated with a decreased risk ( odds ratio 0.57; 95% CI: 0.37- 0.85), on par with other protective factors such as eating fermented foods and being breast fed. Hesselmar’s group previously published a study linking the method of pacifier cleaning with allergy in children. Kids whose parents licked a pacifier clean (mouth cleaning), instead of boiling or tap water cleaning, had fewer allergies. In that previous study, dishwashing of pacifiers was linked with higher allergy risk. Hesselmar’s recent study suggests that machine dishwashing in general may be risky in terms of allergy and asthma risk in children:
 Of course, it remains to be seen if machine dishwashing actually has a causal relationship with allergy, or if it is linked with some other important factor. The authors speculated that hand dishwashing is associated with increased microbial exposure, which has been shown to be protective against allergic diseases. This has been called the hygiene hypothesis – see Weinstock and Elliott 2009 – and Brown et al. 2013 – an idea that has gathered substantial support and refinement as we learn about the role of the microbiome in shaping early immune development.
Of course, it remains to be seen if machine dishwashing actually has a causal relationship with allergy, or if it is linked with some other important factor. The authors speculated that hand dishwashing is associated with increased microbial exposure, which has been shown to be protective against allergic diseases. This has been called the hygiene hypothesis – see Weinstock and Elliott 2009 – and Brown et al. 2013 – an idea that has gathered substantial support and refinement as we learn about the role of the microbiome in shaping early immune development.
Perhaps the most important early microbial exposure is that established by breast milk. Katie Hinde has made this the focus area of her research – read http://science.sciencemag.org/content/348/6242/1427
Dr. Hinde was a keynote speaker at the recent Evolutionary Medicine meeting in Park City Utah. She was joined by Gloria Dominguez Bello who described the importance of birth mode in establishing a beneficial microbiota in children. Read Dr. Dominguez-Bello’s recent work on birth mode and Bifidobacteria here: https://journals.plos.org/plosone/article?id=10.1371/journal.pone.0205962
Much work indicates that early exposures are the most important in being able to modify the risk for autoimmune and inflammatory conditions. Remarkable work in humans links gut microbiota composition with the risk of developing Type 1 diabetes. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4587635/
It is less certain whether microbiome interventions can have a big impact on outcomes in adults. Given the burden of allergic and autoimmune diseases, it makes sense that we should be interested in preventing and treating established disease. This might be best accomplished with diet, and perhaps with probiotics. We will explore these possibilities in Week 2 of the UNM Ev Med Elective.
Categories: Uncategorized
Joe Alcock
Emergency Physician, Educator, Researcher, interested in the microbiome, evolution, and medicine
It’s great news that you’ve been able to get an evolutionary medicine elective into the medical school curriculum! And the hygiene hypothesis is a worthy topic. As you note, it has helped us to make sense of, and potentially prevent and treat, several allergic and autoimmune conditions, which is a feather in the cap of evolutionary medicine. I would like to point out, however, that microbiome disruption probably is not the most important reason for the soaring prevalence of childhood food allergies. In the past 20-25 years, they are up by 50% overall, and they are up by a remarkable 300% in the case of peanuts (US data).
One problem for the hygiene hypothesis (as an explanation for this increase) has to do with timing. Farm-to-city migration, widespread use of antibiotics, and our changing diets—which are thought by many to be the most important sources of microbiome disruption (and throw in automatic dishwashers)—all predate the increase in childhood food allergies by many decades. While it’s possible that a threshold in disruption sufficient to increase food allergies was only reached in the past 20 or so years, that case has not yet been made.
In any event, the hygiene hypothesis has a bigger problem. It can’t explain why childhood food allergies are dramatically reduced by early exposure to allergenic foods. For instance, by eating peanuts while pregnant and breastfeeding, peanut antigen is transferred to the fetus/infant, and the risk of developing a peanut allergy drops dramatically compared to the child of a mother who avoids peanuts while pregnant and nursing. And both children presumably have similarly disrupted microbiomes.
What can explain the protective effect of early introduction of allergenic foods? The mismatch hypothesis I published in Evolutionary Medicine and Public Health in 2017. The gist is that once upon a time, when we were all foragers, our exposure to food antigens as fetuses and infants closely matched the food antigens we were exposed to as we grew older—and our evolving immune system tolerance mechanisms counted on this close match. Modernization, however, produced mismatch, slowly at first with the advent of farming, but then very rapidly about 20-25 years ago, as we entered the so-called ‘age of information.’
Here’s the relevant quote from my article.
“Today, it’s easy to have recipes from far-away places streamed to a mobile device, say from one of the various 24-h food channels, and their ‘exotic’ ingredients also can be easily accessed. This ability to share dietary traditions is unprecedented, and accelerating. . .The problem, with respect to childhood food allergies, is that the mixing of dietary traditions is at a crossroads. Large numbers of people who’ve borrowed widely from the culinary traditions of others live among large numbers of individuals who have remained insular with respect to diet. . .Thus, a child who was not exposed to, for example, peanut or fish proteins during gestation, breastfeeding and in the natal home as an infant and toddler has a far greater chance than even two or three decades ago of being exposed to them downstream, when beginning preschool, kindergarten or just upon being invited to a neighbor’s house for lunch.”
https://academic.oup.com/emph/article/2017/1/154/4344830?guestAccessKey=e4537b85-7222-46a0-a2e2-4a6917d19457
Thanks Paul for these insightful comments
Dr. Alcock, you are providing a great service to our medical society by introducing this type of information into their curriculum. We need more of this type of training. Also, Paul’s explanation is very close to what we observe in swine nutrition and production. We-swine nutritionists and diet formulators-have known for at least 20 years that the timing of exposure of soybean meal for baby pigs before weaning is very important for their subsequent health and performance. In general baby pigs are taken from their mothers at about three weeks of age and it is known that they need a certain quantity of soybean meal consumed before they are weaned to ensure that they respond to normal levels of soybean meal in their diets as they grow and develop. Pigs weaned without adequate intake of soybean meal before weaning never perform at optimal levels later in life. They experience more gastrointestinal problems during the weaning process and elevated levels of morbidity and mortality as they continue to grow. So, even though soybean meal is less digestible than other ingredients such as milk and whey, we add it to our creep diets for the improved later benefits. It is known that the process of introducing the offending ingredient at this early time in the life of the pig improves immune tolerance for the remainder of the pigs life.
Fred Madsen
Fascinating. Thank you Fred. The notion that timing of nutrient introduction has life long effects on development and immune tolerance in particular has important implications for human health.