Over the last 2 years, a wealth of evidence has accumulated supporting the notion that nutrients have predictable effects on the gut microbiota. These observations formed the rationale for our recently published Nutrient Signaling manuscript, published in the Quarterly Review of Biology, with updated observations here.
Moschen and colleagues recently reviewed dietary effects on the microbiota:
(Table 1 “Dietary Factors: Major Regulators of the Gut’s Microbiota” Moschen, Wieser & Tilg. Gut Liver. 2012 Oct;6(4):411-416.)
The modulation of gut microbiota by diet is important because certain nutrients seem to cause an increase in the relative numbers of pathogens and pathobionts. We have proposed that nutrients that increase the numbers of pathogens and pathobionts would be expected to evolve a pro-inflammatory signaling function.
Saturated fat is a key example of a pathogen enhancing nutrient. Devkota and colleagues have recently presented evidence that saturated fat causes blooms of a gram negative Proteobacteria in the gut of mice. A human trial is currently underway.
Omega-6 fatty acids have also recently been identified as a cause of expansion of pathogens and pathobionts ( see Ghosh et al 2013) Ghosh and colleagues write that omega-6 fat “enriched the microbiota with Enterobacteriaceae, Segmented Filamentous Bacteria and Clostridia spp., all known to induce inflammation.”
Omega-3 fatty acids apparently do the opposite, reducing the numbers of inflammation-causing bacteria and reducing translocation of gut bacteria.
These data are in accord with the direct immune effects of these fats. In general, saturated fat and omega-6 confer pro-inflammatory effects. Omega-3 fatty acids are generally anti-inflammatory.
Micronutrients follow the same pattern. For instance, polyphenols in cocoa, citrus, and red wine have each been shown to produce protective changes in microbiota. Nutrients with these effects, if consistent in the human diet over evolutionary time, would be expected to evolve signal characteristics in line with their influence on the microbiota.
I will leave you with an example gleaned from the literature:
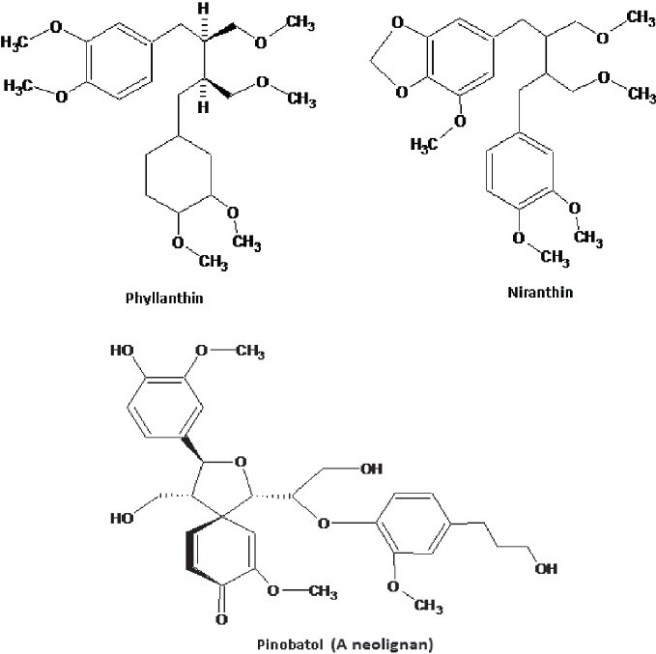
Plant derived alkaloids, glycosides and polyphenols often have anti-diabetic and anti-inflammatory effects. Beg and colleagues have reviewed the immune modulating effects of these compounds which are common in plants and can be found in some foods. Here is an example of a few of these bioactive compounds:
The above polyphenols are derived from the plant Eleutherine americana and show strong anti-inflammatory activity against human macrophages. Eleutherine americana derivatives have been shown to exert a powerful anti-microbial effects against pathogens such as Staphylococcus aureus. (Meanwhile oligosaccharides in the same plant have been shown to promote the growth of beneficial barrier bacteria, such as Lactobacillus.)
A similar concordance of anti-pathogen and anti-inflammatory effects can be seen for a wide variety of these plant compounds. Could their immune activity be an evolutionary consequence of their effects on pathogenic microbes? Alternatively, could these effects represent toxicity to both human and microbial cells? We will explore those competing ideas in a future post.
Categories: Uncategorized
Joe Alcock
Emergency Physician, Educator, Researcher, interested in the microbiome, evolution, and medicine

2 replies ›